The August 2019 update of the Medicaid Vital Signs dashboard continues to examine how the Mississippi Division of Medicaid’s coordinated care organizations (CCOs) have performed in managing certain common disease states among their members. The CCOs are required to report HEDIS data to the Division on a regular basis. HEDIS, which stands for Healthcare Effectiveness Data and Information Set, is a collection of standardized performance measures developed to compare different managed care plans. This month includes additional quality measures related to cardiovascular disease, COPD/asthma and attention deficit hyperactivity disease (ADHD) in children.
At a Glance: Managed Care HEDIS Performance Measures
Cardiovascular Disease
The bar graph above shows the percentages of Medicaid members enrolled with either Magnolia Health Plan or UnitedHealthcare with a diagnosis of cardiovascular disease who were 80% compliant in medication (Statin) adherence during the measurement year.
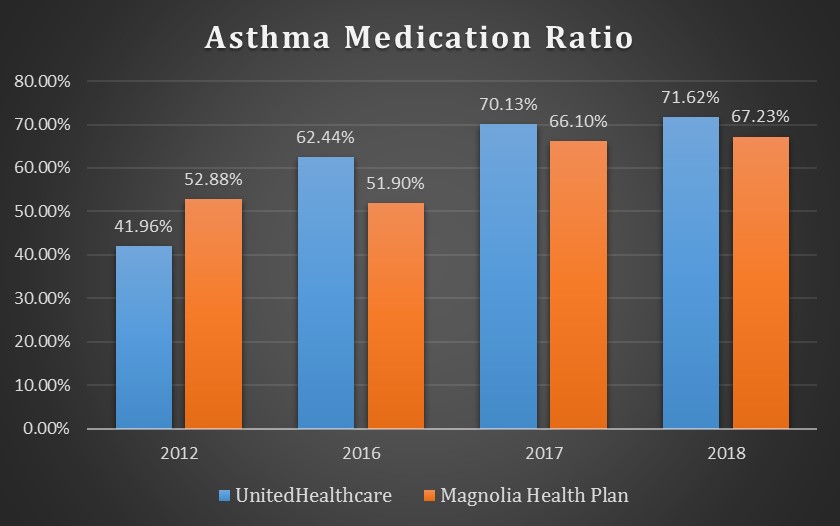
Chronic Obstructive Pulmonary Disease (COPD)/Asthma
The bar graph above shows the percentages of Medicaid members enrolled with either Magnolia Health Plan or UnitedHealthcare with a diagnosis of asthma who had a ratio of controller medications to total asthma medications of 50% or greater (indicating better disease control) during the measurement year.
Attention Deficit Hyperactivity Disease (ADHD)
The bar graph above shows the percentages of Medicaid children enrolled with Magnolia Health Plan between 6 and 12 years of age who had a prescription for ADHD medication and remained on the medication for at least 210 days, and had at least two follow-up visits with a practitioner in the 9 months after the Initiation Phase during the measurement year. (UnitedHealthcare data unavailable.)